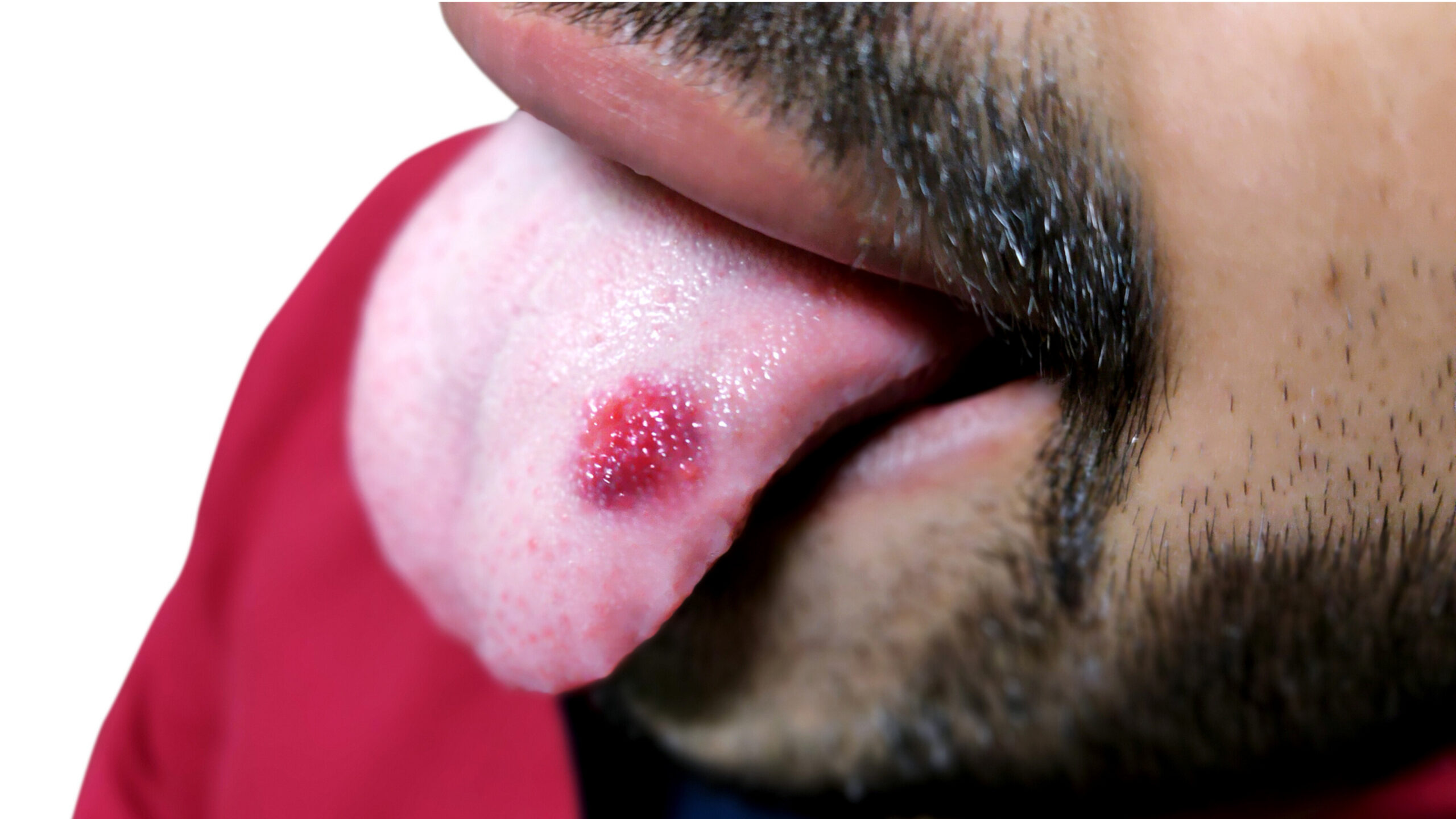
Relief for Oral Lichen Planus in Mouth: Effective Solutions
Oral lichen planus is an autoimmune disorder affecting a notable population segment.
The cause of lichen planus is unknown, but it can lead to discomfort, pain, and scarring in oral mucosa.
This informative article provides a detailed analysis of oral lichen planus, covering its signs, causes, diagnostic processes, treatment alternatives, and potential complications.
In addition, we will delve into how the immune system activates lichen planus and its connection with Hepatitis C infection.
If you or someone close has oral lichen planus, this informative article aims to offer helpful guidance. Keep reading to learn more about Oral Lichen Planus.